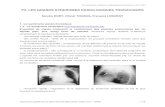
Thrombus muraux thoraciques : Une série et une revue de la littérature
Transcript of Thrombus muraux thoraciques : Une série et une revue de la littérature

Cas clinique
DOI of or1University2University3Harbor-U
CorrespondEast Chestnuthotmail.com
Ann Vasc Surhttp://dx.doi.or� Annals of V�Edit�e par ELS
Thrombus muraux thoraciques : Une s�erieet une revue de la litt�erature
Marvin E. Morris,1 Edgar Luis Gali~nanes,2 W. Kirt Nichols,2 Charles B. Ross,1
Joe Chauvupun,3 Louisville, Kentucky, Columbia, Missouri, et Torrance, California, USA
Les thrombus muraux thoraciques (TMT) sont rares mais une source importante d’emboles dis-taux. Les options de traitement sont vari�ees, allant de la chirurgie ouverte, �a l’endovasculaire,et au traitement conservateur. Nous rapportons deux cas de TMT, un trait�e avec succ�es parstent de l’aorte thoracique pour embolisation visc�erale et p�eriph�erique, et l’autre trait�e demani�ere conservatrice pour embolisation digitale secondaire �a un TMT dans le tronc innomin�e.
Thoracic mural thrombi (TMT) are a rare but impor-
tant source of peripheral emboli. Treatment options
include systemic anticoagulation, surgical throm-
boendarterectomy, resection and replacement with
synthetic conduit, and exclusion with endovascular
stent grafts. We report two cases of TMT, one suc-
cessfully treated with endoluminal stent placement
of a descending thoracic aortic thrombus for persis-
tent infrageniculate embolization. The second
patient presented with hand ischemia from amobile
thrombus in the innominate artery andwas success-
fully treated by anticoagulation therapy.
CASE 1
A 44-year-old, Gravida 2 Para 1, woman with a history
significant for hypertension and menorrhagia requiring
high-dose estrogen therapy presented from an outside
hospital with acute chest and epigastric pain and numb-
ness of her right toes. She was in sinus rhythm. Her
iginal article: 10.1016/j.avsg.2011.05.030.
of Louisville, Louisville, KY, USA.
of Missouri, Columbia, MO, USA.
CLA Medical Center, Torrance, CA, USA.
ance : Marvin E. Morris, University of Louisville, 401Street, Louisville, KY 40059, USA, E-mail: dcmorris12@
g 2011; 25: 1140.e17-1140.e21g/10.1016/j.acvfr.2013.02.007ascular Surgery Inc.EVIER MASSON SAS
abdomen was soft and mildly tender without peritoneal
signs. Her pedal pulses were palpable bilaterally with
motor function intact. Computed Tomography (CT) of the
chest demonstrated an (Fig. 1A) aortic thrombus in the
ascending aorta and a (Fig. 1B) lesion in the mid-
descending thoracic aorta. CT of the abdomen and pelvis
revealed a small amount of free fluid within the pelvis and
focal areas along the small bowel, without evidence of
pneumatosis intestinalis. Findings from CT of the head
were negative. Transesophageal echocardiogram revealed
no evidence of cardiac thrombi. The patient was started on
a systemic heparin and transferred to our facility.
After twelve hours of intravenous unfractionated
heparin, her neurovascular examination changed, with
a loss of pedal pulses, worsening numbness, and decreased
motor function of the right lower extremity. Angiography
revealed emboli in the right tibioperoneal trunk and left
proximal anterior tibialis artery. We focused our efforts
on the descending thoracic lesion as the cause of her pro-
gressing lower extremity symptoms. We excluded the
descending thoracic thrombus with a (Fig. 1C) 116- �24-mm Talent graft. The location of the lesion allowed us
to minimize wire manipulation of the ascending lesion. In
a multidisciplinary decision involving our cardiothoracic
service, her thrombi in the ascending aorta were treated
with systemic anticoagulation. The increased morbidity
and mortality, a surgical intervention, and the anatomic
complexity of an endovascular approach dictated our
therapeutic algorithm. After stent deployment, the peri-
pheral emboli in her legs were treated with catheter-
directed thrombolysis for 24 hours.
Interval angiography demonstrated resolution of her
embolic lesions with good runoff bilaterally. Her pedal
pulses were again palpable. Systemic anticoagulation
with heparin was converted to warfarin with a target
1214.e17

Fig. 1. (A) Thrombus in the ascending aorta. (B) Thrombus in the mid-descending aorta. (C) Endovascular graft
covering the descending aorta.
1214.e18 Cas cliniques Annales de chirurgie vasculaire
international normalized ratio (INR) of 2-3. Her symp-
toms resolved and findings from hypercoagulability panel
were negative. A gynecologist was consulted for her
menorrhagia, and she was started on IM Depo-Provera.
She continued to do well and was discharged to home
on postoperative day 7 with close surveillance.
CASE 2
A 43-yeareold woman, who is a former 1.5-pack-per-day
smoker, with a history of diabetes mellitus, hypertension,
and menorrhagia was transferred with progressive ische-
mic pain and discoloration of the fingers of the right hand
over the course of 2 weeks. On presentation, she was in
sinus rhythm, with equal blood pressure in both upper
extremities and with palpable pulses in the ulnar and
radial arteries bilaterally. Cyanotic discoloration was
prominently noted in all five fingers of the right hand,
more pronounced in fingers 2-5. Ischemic changes in
these digits extended proximally to proximal inter-
phalangeal joint levels, with the fingers being cold and
painful to touch and movement (Fig. 2A). History was
negative for antecedent collagen vascular disorders, vas-
culitis, and thrombophilias. Home medications included
metformin, byetta, and a thiazide diuretic. Pertinent
laboratory findings included a platelet count of 499;
erythrocyte sedimentation rate was mildly elevated at 50.
A presumptive diagnosis of Reynaud syndrome was
entertained, and she was started on Methylprednisolone.
A transthoracic echocardiogram was negative for atrial
thrombus and cardiac valvular anomalies. CT angiogram
(CTA) revealed a large thrombus in the innominate artery
(Fig. 2B). Anticoagulation therapy was initiated with
unfractionated heparin infusion, and within 24 hours,
there was resolution of her hand cyanosis. Warfarin was
initiated with a target INR of 2.0-3.0. One year later, her
index finger was persistently cyanotic, but her remaining
digits were normal (Fig. 2C). Follow-up CTA revealed
resolution of her innominate artery thrombus (Fig. 2D).
She remains anticoagulated with warfarin with an INR
of 2-3.
DISCUSSION
TMT is an intriguing pathology with a dynamic the-
rapeutic armamentarium. TMT is increasingly
recognized as a source of peripheral emboli, either
to the viscera, cerebrovascular circulation, or most
commonly the lower extremities. TMT characterizes
an aortic thrombus in the ascending aorta or its
branches or the descending aorta, typically in young
people, in the absence of preexisting disease.1 Aortic
thrombus of the thoracic aorta most commonly
occurs in the transverse aortic arch with a pre-
dilection for the aortic isthmus and is often limited
to a focal lesion. This distinguishes all forms of
TMT from other atherosclerotic lesions, which are
traditionally found diffusely distributed throughout
the arterial system.2-6 Risk factors include younger
age, smoking, and a family history of athero-
sclerosis. The majority of reported cases have been

Fig. 2. (A) Cyanosis of the distal right hand. (B) Innominate artery thrombus. (C) Resolution of innominate artery
thrombus. (D) Resolution of cyanosis of distal right hand.
Vol. 25, No. 8, 2011 Cas cliniques 1214.e19
diagnosed after an embolic event. Currently
unknown, the pathophysiology is multifactorial;
theories include thrombophilias secondary to mali-
gnancy, and exogenous steroids use.1,2 Both our
patients had no definable thrombophilias, no ante-
cedent history of steroid use, and no evidence of
malignancy.
Mobile thrombi originating from the innominate
artery are extremely rare. Based on the limited am-
ount of literature, any recommendations on theman-
agement of innominate artery thrombus have to be
extrapolated from AMT. Innominate artery thrombi
clinically manifest as cerebrovascular events, digital
ischemia, arm fatigue, and angina.1,2 Anatomically,
tracheal interposition and atheromatous disease may
preclude diagnosis with transesophageal echocar-
diography (TEE). Gadolinium-enhanced magnetic
resonance angiogram (MRA) may provide complete
visualizations of the arch vessels, including the
innominate artery, in cases of normal TEEwith a high
clinical suspicion for right-sided embolic sources.
False-positive images due to circulatory turbulence
have been reported.1 CTA is now considered the
diagnostic modality of choice for operative planning.
In both of our cases, CTA was diagnostic and negated
the need for invasive angiography, which can be
catastrophic owing to the risk of thrombus migration
and embolization.7-9

1214.e20 Cas cliniques Annales de chirurgie vasculaire
Treatment algorithm is controversial; therefore,
there is no consensus for the appropriate therapeutic
regimen for TMT. Therapeutic options include
anticoagulation,2,10 thrombolysis,11 thromboaspira-
tion,12 open thromboendarterectomy, and exclusion
using endoluminal stent grafts. In general, a trial of
anticoagulation is pursued, with surgical repair or
endovascular intervention reserved for patients who
fail to respond. Persistence of a mass by TEE after
anticoagulation or highly mobile appearance of the
thrombus may lead to operative intervention. Sur-
gical options include thrombectomywith or without
resection of the atherosclerotic plaque, with repair of
the aorta using either Dacron or polytetrafluoroe-
thylene. In a contemporary series of nine cases of
TMT by Chakroun et al., 50% of patients had failure
of medical therapy, requiring surgical intervention;
Goueffic treated 38 patients with open surgical
techniques, with a mortality of 2.6%.1
Recurrence is a major issue with TMT, and long-
term anticoagulation is recommended. In the study
by Patra et al., recurrence was observed in 27% of
patients treated medically, typically in remote ana-
tomical locations. Recurrence after surgical repair
has been reported.3,4 Our initial patient was treated
with thoracic stent graft owing to progressive sym-
ptomatology and limb threat, and our second patient
received full anticoagulationwith an unfractionated
heparin bridge to warfarin. A subsequent CTA in 4
weeks showed complete resolution of her thrombus.
The discoloration of her hand took weeks to resolve,
but she is fully functionalwithout residual deficits or
further embolic events to date at 1-year follow-up.
The use of endovascular devices to treat sym-
ptomatic aortic pathology allows exclusion of the
plaque from the circulation while separating the
intima from rheological factors that may promote
platelet deposition and further embolization.13-18
Various case reports in the literature describe the use
of stent grafts as sole treatment or in conjunction
with other treatment options in the management of
thoracic mural thrombi. Our first case adds to the
body of literature supporting use of thoracic aortic
stent grafts to treat AMT.
Transluminal balloon angioplasty and stenting
has become the preferred method for management
of primary atherosclerotic lesions of the innominate
artery owing to a greater than 90% initial success
and limited morbidity. Long-term follow-up data
for treatment of atherosclerotic lesions are currently
not available.19-27 Although exclusion of mobile
thrombus in the innominate artery by stent grafting
is feasible by endoluminal techniques, experience is
limited. Because of the risk of embolization, open
exposure of the common carotid artery and clamping
with retrograde treatment of the innominate lesion,
complete with thorough flushing before closure,
would seem prudent. This technique has been
reported formanagement of standard atherosclerotic
lesions with favorable outcomes.15 For lesions
located at the origin of the innominate with invol-
vement of the ascending aorta, open thromboen-
darterectomy facilitated by circulatory arrest may be
required. Morbidity and mortality in these cases
can approximate 30%.1 Although data are anec-
dotal, as in our second case, a trial of anticoagulation
therapy seems practical, with more aggressive
interventions reserved for treatment failure.
Endovascular stenting for lesions in the ascend-
ing aorta has been reported in small series of
patients. Arch anatomy and configuration (whether
conical or tubular) in the cases of treatment of aneu-
rysmal pathology dictate treatment plan and suc-
cess. Important tenants of proper device placement
include the use of fixation with hooks, the appro-
priate oversizing, and caution not to compromise
aortic valve closure. A mismatch between the inner
and outer curvatures of the ascending aorta may
result in kinking of the stent graft.28 Temporary
cardiac arrest, rapid ventricular overpacing, and
partial atrial inflow occlusion to induce controlled
hypotension have been advocated to achieve suc-
cessful graft deployment.29-31 These anatomical
constraints limit aortic arch endovascular stenting to
high-risk surgical patients unfit for open repair.
In conclusion, TMT is a dynamic pathological
process with evolving therapeutic options. High cli-
nical suspicion is needed for diagnosis, and patient
care should be individualized with an emphasis
toward minimizing morbidity and mortality. The
use of aortic stent graft technology provides a mini-
mally invasive approach to treat this complex path-
ology. Innominate artery mobile thrombus (IAMT)
presents additional therapeutic dilemmas, with
anticoagulation representing a viable option for
management. Long-term anticoagulation therapy,
optimization of atherosclerotic risk factors, and
surveillance are essential because all available
treatment modalities may initially fail or be com-
plicated by late recurrence.
REFERENCES
1. Choukran EM, Labrousse LM, Madonna FP, Deville C.
Mobile thrombus of the thoracic aorta: diagnosis and treat-
ment in 9 cases. Ann Vasc Surg 2002;16:714-722.
2. Bowdish M, Weaver F, Leibman H, et coll. Anticoagulation
is an effective treatment for aortic mural thrombi. J Vasc
Surg 2002;36:713-719.
3. Patra P, Pilllet JC, Chaillou P, Duveau D. Traitement chi-
rurgical des lCsions emboligknes de la crosse de l’aorte. Paris:
Pharmapost, 1997. pp 11-31.

Vol. 25, No. 8, 2011 Cas cliniques 1214.e21
4. Laperche T, Laurian C, Roudant R, et coll. Mobile thromboses
of the aortic arch without aortic debris: a transesophageal
echocardiographic finding associated with unexplained arte-
rial embolism. Circulation 1997;96:288-294.
5. Mitchell MM, Frankville DD, Weinger MB, Dittrich HC.
Detection of thoracic aortic atheroma with transesophageal
echocardiography in patients without symptoms of embo-
lism. Am Heart J 1991;122:1768-1771.
6. Tunick PA, Perez JC, Kronzon I. Protruding atheromas in
the thoracic aorta and systemic embolization. Ann Intern
Med 1991;115:423-427.
7. Cohen A, Chauvel C, Abergel E, et coll. Interst de I’echo-
cardiographie transocsophagicnne dans le bilan cardio-
vasculaire d’un accident ischemique cerebral presume
d’origine embolique. Ann Radiol 1994;37:29-40.
8. Karalis DG, Chandrasekaran K, Victor MF, et coll. Reco-
gnition and embolic potential of intraaortic atherosclerotic
debris. J Am Coll Cardiol 1991;17:73-78.
9. Dee W, Geibel A, Kasper W, et coll. Mobile thrombi in
atherosclerotic lesions of the thoracic aorta: the diagnostic
impact of transesophageal echocardiography. Am Heart J
1993;126:707-710.
10. Hausmann D, Gulba D, Bargheer K, et coll. Successful
thrombolysis of an aortic arch thrombus in a patient after
mesenteric embolism. N Engl J Med 1992;327:500-501.
11. Reber PU, Patel AG, Stauffer E, et coll. Mural aortic thrombi:
an important cause of peripheral embolization. J Vasc Surg
1999;30:1084-1089.
12. Goueffic Y, Chaillou P, Pillet JC, Duveau D, Patra P. Surgical
treatment of nonaneurysmal aortic lesions in patients
with systemic embolization. J Vasc Surg 2002;36:1186-1193.
13. Modrai B, Ali R, Dourado J, et coll. Comparison of extra-
anatomic bypass grafting with angioplasty for athero-
sclerotic disease of the supra-aortic trunks. Br J Surg 2004;
91:1453-1457.
14. Shames ML, Rubin B, Sanchez L, et coll. Treatment of
embolizing arterial lesions with endoluminally placed stent
grafts. Ann Vasc Surg 2002;16:608-612.
15. Queral LA, Criado FJ. The treatment of focal aortic arch
branch lesions with Palmaz stents. J Vasc Surg 1996;23:
368-375.
16. Piffaretti G, Tozzi M, Caronno R, Castelli P. Endovascular
treatment for mobile thrombus of the thoracic aorta. Eur J
Cardiothorac Surg 2007;32:664-667.
17. Luebke T, Aleksic M, Brunkwall J. Endovascular therapy of
a symptomatic mobile thrombus of the thoracic aorta. Eur J
Vasc Endovasc Surg 2008;36:550-552.
18. Luckeroth P, Steppacher R, Rohrer MJ, Eslami MH. Endo-
vascular therapy for symptomatic mobile thrombus of
infrarenal abdominal aorta. Vasc Endovasc Surg 2009;43:
518-523.
19. Fueglistaler P, Wolff T, Guerke L, Stierli P, Eugster T.
Endovascular stent graft for symptomatic mobile thrombus
of the thoracic aorta. J Vasc Surg 2005;42:781-783.
20. Huttl K, Nemes B, Simonffy A, Entz L, Berzci V. Angio-
plasty of the innominate artery in 8 patients: experience
over 19 years. Cardiovasc Intervent Radiol 2002;25:
109-114.
21. Deitrich EB. Endovascular management of brachiocephalic
arterial occlusive disease. Ann Vasc Surg 2000;14:189-192.
22. Ruebben A, Tettoni S, Muratore P, et coll. Feasibility of
intraoprative balloon angioplasty and additional stent pla-
cement of isolated stenosis of the brachiocephalic trunk.
J Thorac Cardiovasc Surg 1998;115:1316-1320.
23. Sullivan TM, Gray BH, Bacharach, et coll. Angioplasty and
primary stenting of the subclavian, innominate and com-
mon carotid arteries in 83 patients. J Vasc Surg 1998;28:
1059-1065.
24. Greenberg RK, Waldman D. Endovascular and open surgical
treatment of brachiocephalic arterial disease. Semin Vasc
Surg 1998;11:77-90.
25. Craido FJ, Twena M. Techniques for endovascular recana-
lization of supra-aortic trunks. J Endovasc Surg 1996;4:
405-413.
26. Kesheva SN, Falk A. Revascularization of aortic arch
branches and visceral arteries using minimally invasive
endovascular techniques. Mt Sinai J Med 2003;70:
401-409.
27. Brountzas EN, Petersen B, Binkert C, et coll. Primary
stenting of subclavian and innominate artery occlusive
disease: a single center’s experience. Cardiovasc Intervent
Radiol 2004;27:616-623.
28. Kolvenbach R, Karmelli R, Pinter L, et coll. Endovascular
management of ascending aortic pathology. J Vasc Surg
2011;53:1431-1437.
29. Lee WA. Partial right atrial inflow occlusion for TEVAR.
Endovasc Today 2009;10:39-44.
30. Lee WA, Martin T, Gravenstein N. Partial right atrial inflow
occlusion for controlled systemic hypotension during tho-
racic endovascular aortic repair. J Vasc Surg 2008;48:
494-498.
31. Lee WA, Martin TD, Hess PJ, Beaver TM, Huber TS. Mal-
deployment of the TAG thoracic endograft. J Vasc Surg
2007;46:1032-1035.